Items filtered by date: March 2022
Heel Pain Can Be Treated!
Foot Problems and Falling as We Age
 Foot problems can lead to pain, swelling, numbness and tingling of feet. These symptoms can come from blisters, bunions, heel spurs, diabetes complications, hammertoes, and the like. Regardless of the cause, foot problems can impact balance and gait and contribute to falls. The elderly population is more vulnerable when it comes to foot problems and resultant falls. Simple walking impacts bones, joints, muscles, ligaments, and tendons and the longer we live, the more wear and tear on feet. As we age, padding on the bottom of the feet wears off, arches become flatter and less flexible, and ankles and joints become stiff. Feet even become wider and longer as we age. Pre-existing physical conditions impacting feet and ankles, like heart and vascular disease and kidney disease, puts one at greater risk for foot problems as well. All these natural changes can lead to foot pain and problems, such as arthritis and gout and increase the propensity for falling. Proper care of feet and regular exercise, with a focus on lower body strengthening, are important as we grow older. Regular consultation with a podiatrist can help one maintain foot health and prevent complications leading to falls as we age.
Foot problems can lead to pain, swelling, numbness and tingling of feet. These symptoms can come from blisters, bunions, heel spurs, diabetes complications, hammertoes, and the like. Regardless of the cause, foot problems can impact balance and gait and contribute to falls. The elderly population is more vulnerable when it comes to foot problems and resultant falls. Simple walking impacts bones, joints, muscles, ligaments, and tendons and the longer we live, the more wear and tear on feet. As we age, padding on the bottom of the feet wears off, arches become flatter and less flexible, and ankles and joints become stiff. Feet even become wider and longer as we age. Pre-existing physical conditions impacting feet and ankles, like heart and vascular disease and kidney disease, puts one at greater risk for foot problems as well. All these natural changes can lead to foot pain and problems, such as arthritis and gout and increase the propensity for falling. Proper care of feet and regular exercise, with a focus on lower body strengthening, are important as we grow older. Regular consultation with a podiatrist can help one maintain foot health and prevent complications leading to falls as we age.
Preventing falls among the elderly is very important. If you are older and have fallen or fear that you are prone to falling, consult with Matthew McQuaid, DPM from Lake Mendocino Podiatry. Our doctor will assess your condition and provide you with quality advice and care.
Every 11 seconds, an elderly American is being treated in an emergency room for a fall related injury. Falls are the leading cause of head and hip injuries for those 65 and older. Due to decreases in strength, balance, senses, and lack of awareness, elderly persons are very susceptible to falling. Thankfully, there are a number of things older persons can do to prevent falls.
How to Prevent Falls
Some effective methods that older persons can do to prevent falls include:
- Enrolling in strength and balance exercise program to increase balance and strength
- Periodically having your sight and hearing checked
- Discuss any medications you have with a doctor to see if it increases the risk of falling
- Clearing the house of falling hazards and installing devices like grab bars and railings
- Utilizing a walker or cane
- Wearing shoes that provide good support and cushioning
- Talking to family members about falling and increasing awareness
Falling can be a traumatic and embarrassing experience for elderly persons; this can make them less willing to leave the house, and less willing to talk to someone about their fears of falling. Doing such things, however, will increase the likelihood of tripping or losing one’s balance. Knowing the causes of falling and how to prevent them is the best way to mitigate the risk of serious injury.
If you have any questions, please feel free to contact our offices located in Lakeport and Ukiah, CA . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Have I Sprained My Ankle?
Ankle sprains are a fairly common injury to the rubber band-like ligaments that connect and hold the ankle bones together. Not all ankle sprains are the same. Severity depends upon how many ligaments are affected, and whether they are overly stretched, or partially/fully torn. Having weak ankles, running on uneven surfaces, playing sports, wearing inappropriate shoes, and having prior ankle sprains can increase a person’s risk of spraining their ankle. Along with pain, an ankle sprain may cause bruising, swelling, stiffness, soreness and even difficulty walking. If your ankle does not heal properly, it could lead to future ankle sprains and chronic ankle instability. Sometimes an ankle sprain will occur along with another type of foot or ankle injury that should be addressed as well. To avoid these problematic situations, contact a podiatrist if you believe you have sprained your ankle.
Ankle sprains are common but need immediate attention. If you need your feet checked, contact Matthew McQuaid, DPM from Lake Mendocino Podiatry. Our doctor can provide the care you need to keep you pain-free and on your feet.
How Does an Ankle Sprain Occur?
Ankle sprains take place when the ligaments in your ankle are torn or stretched beyond their limits. There are multiple ways that the ankle can become injured, including twisting or rolling over onto your ankle, putting undue stress on it, or causing trauma to the ankle itself.
What Are the Symptoms?
- Mild to moderate bruising
- Limited mobility
- Swelling
- Discoloration of the skin (depending on severity)
Preventing a Sprain
- Wearing appropriate shoes for the occasion
- Stretching before exercises and sports
- Knowing your limits
Treatment of a Sprain
Treatment of a sprain depends on the severity. Many times, people are told to rest and remain off their feet completely, while others are given an air cast. If the sprain is very severe, surgery may be required.
If you have suffered an ankle sprain previously, you may want to consider additional support such as a brace and regular exercises to strengthen the ankle.
If you have any questions please feel free to contact our offices located in Lakeport and Ukiah, CA . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Why Is Duplex Ultrasound Used to Diagnose PAD?
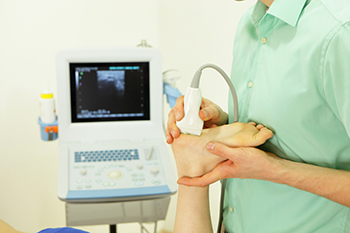
If your podiatrist suspects that you may have peripheral artery disease (PAD), they will most likely perform a vascular test called a duplex ultrasound. Duplex ultrasound uses two modes of ultrasound: 1) traditional ultrasound to create images of your blood vessels based on sound waves bouncing off them, and 2) doppler ultrasound to estimate the speed and direction of blood by recording sound waves that reflect off it as it flows. Duplex ultrasound is non-invasive and painless. Your podiatrist will spread gel on the skin of the area(s) to be tested, and then wave a transducer wand which emits the sound waves and records the echoes that are reflected. For more information about duplex ultrasound, ask your podiatrist.
Vascular testing plays an important part in diagnosing disease like peripheral artery disease. If you have symptoms of peripheral artery disease, or diabetes, consult with Matthew McQuaid, DPM from Lake Mendocino Podiatry. Our doctor will assess your condition and provide you with quality foot and ankle treatment.
What Is Vascular Testing?
Vascular testing checks for how well blood circulation is in the veins and arteries. This is most often done to determine and treat a patient for peripheral artery disease (PAD), stroke, and aneurysms. Podiatrists utilize vascular testing when a patient has symptoms of PAD or if they believe they might. If a patient has diabetes, a podiatrist may determine a vascular test to be prudent to check for poor blood circulation.
How Is it Conducted?
Most forms of vascular testing are non-invasive. Podiatrists will first conduct a visual inspection for any wounds, discoloration, and any abnormal signs prior to a vascular test.
The most common tests include:
- Ankle-Brachial Index (ABI) examination
- Doppler examination
- Pedal pulses
These tests are safe, painless, and easy to do. Once finished, the podiatrist can then provide a diagnosis and the best course for treatment.
If you have any questions, please feel free to contact our offices located in Lakeport and Ukiah, CA . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Read more about Vascular Testing in Podiatry
Can Cracked Heels Be Prevented?
 The foot condition known as cracked heels can develop for several reasons. These can include a vitamin deficiency, being overweight, and certain fungal conditions. Additionally, people who are diabetic may be more likely to experience cracked heels. This may be a result from a lack of circulation that can often accompany diabetes. Fissures, which are deep cracks in the skin, can cause significant pain and discomfort. Relief may be found when shoes that are worn have a closed back. Additionally, patients have found their skin may soften when a good moisturizer is applied, and it may help to avoid being barefoot. Drinking plenty of fresh water daily may help to reduce the risk of developing cracked heels. If you would like more information about how to prevent the onset of cracked heels, please confer with a podiatrist who can provide you with proper knowledge.
The foot condition known as cracked heels can develop for several reasons. These can include a vitamin deficiency, being overweight, and certain fungal conditions. Additionally, people who are diabetic may be more likely to experience cracked heels. This may be a result from a lack of circulation that can often accompany diabetes. Fissures, which are deep cracks in the skin, can cause significant pain and discomfort. Relief may be found when shoes that are worn have a closed back. Additionally, patients have found their skin may soften when a good moisturizer is applied, and it may help to avoid being barefoot. Drinking plenty of fresh water daily may help to reduce the risk of developing cracked heels. If you would like more information about how to prevent the onset of cracked heels, please confer with a podiatrist who can provide you with proper knowledge.
If the skin on your feet starts to crack, you may want to see a podiatrist to find treatment. If you have any concerns, contact Matthew McQuaid, DPM from Lake Mendocino Podiatry. Our doctor can provide the care you need to keep you pain-free and on your feet.
Cracked Heels
It is important to moisturize your cracked heels in order to prevent pain, bleeding, and infection. The reason cracked heels form is because the skin on the foot is too dry to support the immense pressure placed on them. When the foot expands, the dry skin on the foot begins to split.
Ways to Help Heal Them
- Invest in a good foot cream
- Try Using Petroleum Jelly
- Ease up on Soaps
- Drink Plenty of Water
Ways to Prevent Cracked Heels
- Moisturize After Showering
- Skip a Shower
- Keep Shower Water Lukewarm
- Don’t Scrub Your Feet
If you are unsure how to proceed in treating cracked heels, seek guidance from a podiatrist. Your doctor will help you with any questions or information you may need.
If you have any questions, please feel free to contact our offices located in Lakeport and Ukiah, CA . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Types of Metatarsal Fractures
 The metatarsals are the five long bones located in the middle of your foot which connect the toes to the rest of the foot. When any of these bones break, it is known as a metatarsal fracture. There are several types of metatarsal fractures. Stress fractures occur when a bone develops one or more tiny cracks due to it being unable to bear the load placed on it. A Lisfranc fracture-dislocation occurs when the second metatarsal bone is broken and knocked out of place. A fracture of the fifth metatarsal bone, the most common type of metatarsal fracture, occurs when excessive stress or overuse causes the bone that connects your pinky toe to the rest of your foot to break. If you have symptoms of a broken foot bone, such as pain, swelling, bruising, and difficulty walking or bearing weight on the injured foot, it is strongly suggested that you seek the care of a podiatrist as soon as possible.
The metatarsals are the five long bones located in the middle of your foot which connect the toes to the rest of the foot. When any of these bones break, it is known as a metatarsal fracture. There are several types of metatarsal fractures. Stress fractures occur when a bone develops one or more tiny cracks due to it being unable to bear the load placed on it. A Lisfranc fracture-dislocation occurs when the second metatarsal bone is broken and knocked out of place. A fracture of the fifth metatarsal bone, the most common type of metatarsal fracture, occurs when excessive stress or overuse causes the bone that connects your pinky toe to the rest of your foot to break. If you have symptoms of a broken foot bone, such as pain, swelling, bruising, and difficulty walking or bearing weight on the injured foot, it is strongly suggested that you seek the care of a podiatrist as soon as possible.
A broken foot requires immediate medical attention and treatment. If you need your feet checked, contact Matthew McQuaid, DPM from Lake Mendocino Podiatry. Our doctor can provide the care you need to keep you pain-free and on your feet.
Broken Foot Causes, Symptoms, and Treatment
A broken foot is caused by one of the bones in the foot typically breaking when bended, crushed, or stretched beyond its natural capabilities. Usually the location of the fracture indicates how the break occurred, whether it was through an object, fall, or any other type of injury.
Common Symptoms of Broken Feet:
- Bruising
- Pain
- Redness
- Swelling
- Blue in color
- Numbness
- Cold
- Misshapen
- Cuts
- Deformities
Those that suspect they have a broken foot shoot seek urgent medical attention where a medical professional could diagnose the severity.
Treatment for broken bones varies depending on the cause, severity and location. Some will require the use of splints, casts or crutches while others could even involve surgery to repair the broken bones. Personal care includes the use of ice and keeping the foot stabilized and elevated.
If you have any questions please feel free to contact our offices located in Lakeport and Ukiah, CA . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.